Bone Marrow Edema: Causes, Symptoms, and Treatment
Bone health is a fundamental factor that directly affects quality of life and mobility. Today, many people face various bone issues, especially in weight-bearing areas. One of the most common of these problems is bone marrow edema. Bone marrow edema is characterized by fluid accumulation within the bone tissue and is a frequently encountered condition. It typically occurs in weight-bearing joints such as the knees, hips, ankles, and spine. These areas are constantly exposed to pressure and strain during daily activities.
Patients with bone marrow edema may experience severe pain, tenderness, and limited mobility. This leads to a significant decrease in quality of life. However, with early diagnosis and proper treatment approaches, symptoms can be effectively managed.
In this article, we will comprehensively cover all important details about bone marrow edema. By accessing accurate information, you can increase your awareness and better protect your bone health.
Table of Contents
- What Is Bone Marrow Edema?
- What Causes Bone Marrow Edema?
- What Are the Symptoms of Bone Marrow Edema?
- How Is Bone Marrow Edema Diagnosed?
- Which Treatment Options Are Effective for Bone Marrow Edema?
- The Role of Exercise and Physical Therapy in Bone Marrow Edema
- How Is Bone Marrow Edema Treated?
- Frequently Asked Questions
- Conclusion
What Is Bone Marrow Edema?
Bone marrow edema is a significant health issue that occurs when fluid accumulates within the bone tissue and is commonly seen in many individuals. This fluid fills the microscopic spaces within the spongy structure of the bone. Over time, it creates pressure on the surrounding tissues. As the pressure increases, pain, tenderness, and discomfort during movement arise. These effects are particularly noticeable in weight-bearing joints.
In medical literature, bone marrow edema is not classified as a standalone disease. Instead, it is generally considered a sign or result of an underlying orthopedic or systemic problem.
Sprains, fractures, bone marrow disorders, circulatory issues, or rheumatic diseases can contribute to the development of bone marrow edema. Therefore, making an accurate diagnosis is critically important for initiating an effective treatment process. If not detected early and properly treated, bone marrow edema may lead to serious disabilities and long-term mobility limitations. In chronic cases, it can even result in permanent loss of function in daily activities.
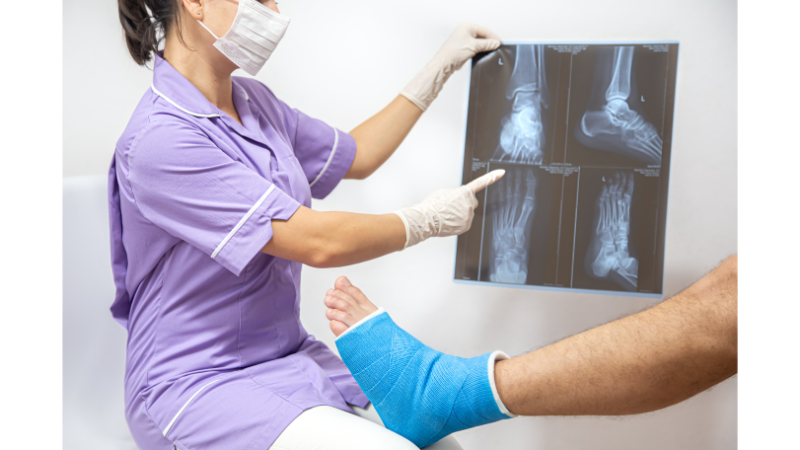
What Causes Bone Marrow Edema?
Many different factors can contribute to the development of bone marrow edema. Trauma is one of the most significant causes. Falls, impacts, sports injuries, and various accidents can cause micro-level damage within the bone tissue. These minor injuries create conditions for fluid accumulation in the spongy structure of the bone. Over time, this leads to bone marrow edema.
In addition to physical trauma, several systemic and degenerative diseases also play a role in its development. Overloading and repetitive stress place constant pressure on the bone, which can damage the tissue. Osteoarthritis, which refers to the gradual wear and deterioration of joint cartilage, is one of the most common causes of bone marrow edema.
Rheumatic diseases may also trigger inflammation and fluid accumulation in bone tissue through the immune system. Circulatory disorders are another significant risk factor. In conditions such as avascular necrosis, blood supply to the bone becomes insufficient. This leads to nutritional deficiencies in the bone tissue. As a result, edema can develop.
Certain infections can cause inflammatory reactions in the bone, contributing to the formation of edema. In addition, bone tumors and cysts may create conditions that allow fluid to accumulate within the bone. Long-term use of corticosteroids and certain medications can weaken bone tissue and increase the risk of edema.
Athletes and individuals who engage in intense physical activity are more prone to developing bone marrow edema. Constant strain and overuse can lead to micro-damage in the bone tissue. In older adults, decreased bone density, increased joint load due to obesity, and metabolic diseases such as diabetes significantly raise the risk of developing bone marrow edema. Detecting and controlling these risk factors at an early stage is critically important for preventing potential complications.
What Are the Symptoms of Bone Marrow Edema?
- Bone marrow edema may cause persistent pain, even while resting. Over time, this pain can become more severe.
- Swelling and tenderness often develop in the affected area.
- Joint movements may become restricted. As mobility decreases, flexibility is also reduced.
- Pain intensifies when weight is applied to the affected area or when pressure is exerted.
- In prolonged cases, muscle weakness and a general feeling of fatigue may occur.
- The severity of pain varies depending on the size of the edema and the underlying cause.
- The knees, hips, and ankles are the most commonly affected joints. Edema in these regions can interfere with daily activities and significantly lower the quality of life.
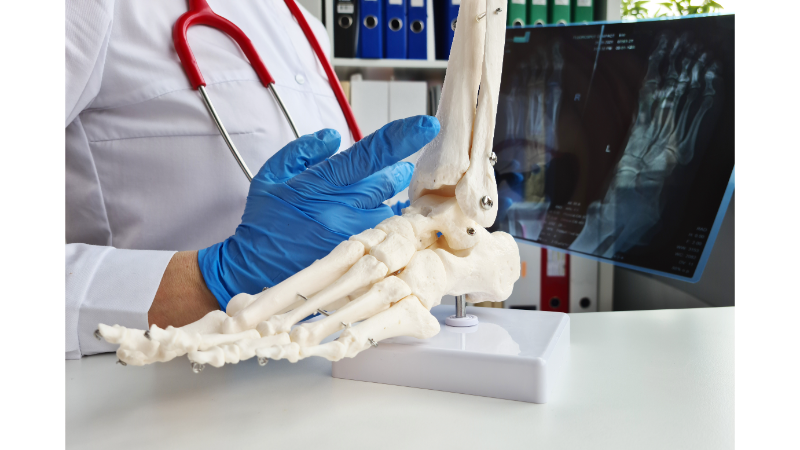
How Is Bone Marrow Edema Diagnosed?
- Magnetic Resonance Imaging (MRI):
MRI is the most effective method for diagnosing bone marrow edema. It clearly and precisely shows fluid accumulation within the bone tissue. MRI provides definitive information about the location, size, and extent of the edema. - Physical Examination:
The physician carefully examines the area where the patient experiences pain. Tenderness, swelling, limited range of motion, and pain upon pressure are assessed. - Detailed Medical History:
Information is gathered about past traumas, previous illnesses, medications used, and lifestyle factors. This plays an important role in identifying underlying causes. - Blood Tests:
Blood work is performed to investigate infections, inflammation, rheumatic diseases, and metabolic disorders. Certain systemic conditions may contribute to the development of bone marrow edema. - X-Ray (Direct Radiography):
X-rays are used especially when fractures are suspected. Structural changes, fractures, or degenerative alterations in the bone can be visualized. - Comprehensive Evaluation:
All test results and clinical findings are evaluated together to establish a definitive diagnosis. An accurate diagnosis allows for the creation of an effective treatment plan.
Which Treatment Options Are Effective for Bone Marrow Edema?
With advancements in medical technology, several innovative treatment methods have been introduced in recent years. These methods have proven effective, especially in advanced cases of edema and situations where standard treatments are insufficient.
PRP (Platelet-Rich Plasma) therapy is one of the significant innovations in this field. Platelet-rich plasma, obtained through special processing of the patient’s own blood, is injected directly into the affected area. The growth factors contained in the platelets enhance the tissue’s self-repair capacity. This application accelerates tissue healing and may also reduce the inflammatory process.
Shock Wave Therapy (ESWT) is another increasingly preferred option for treating bone marrow edema. In this method, focused high-frequency sound waves are directed to the area of edema. These sound waves improve blood circulation in the region, promoting cell nutrition and repair. As a result, the healing process is accelerated, and pain symptoms can significantly decrease.
Physical therapy also plays an important role in managing bone marrow edema. Special exercise programs are designed to help patients maintain muscle strength and joint range of motion. Additionally, supportive methods such as electrotherapy, ultrasound, laser therapy, and hot-cold applications are included in the physical therapy protocol. These treatments contribute to the reduction of edema and improve the patient’s functional capacity.
In rare and advanced cases, surgical intervention may become necessary. Especially in conditions such as avascular necrosis, where the bone tissue is severely damaged, surgical options are considered. Surgical procedures may involve cleaning the damaged tissues or, when necessary, planning joint prosthesis applications.
The Role of Exercise and Physical Therapy in Bone Marrow Edema
When performed correctly, exercise and physical therapy make significant contributions to the healing process of bone marrow edema. Controlled and properly guided exercises not only help reduce the edema but also maintain the patient’s overall muscle and joint health. Exercise programs must always be designed under expert supervision and tailored to the patient’s specific condition.
Physical therapy helps prevent muscle atrophy, which refers to muscle wasting that can occur during periods of inactivity. Without movement, muscles begin to weaken. Regular physical therapy keeps the muscle tissue active and prevents strength loss. At the same time, joint mobility is preserved. Appropriate exercises are planned to prevent joint stiffness and loss of range of motion.
Physical therapy programs also have positive effects on pain management. Supportive methods such as electrotherapy, ultrasound, hot-cold applications, and laser therapy help reduce pain. This enables patients to participate more comfortably in daily activities. Preserving and improving functional capacity is one of the main goals of physical therapy.
However, during the early stages of treatment, overloading and unsupervised exercises must be strictly avoided. Incorrect or untimely exercises may worsen the existing edema and prolong the recovery period. Therefore, every exercise program must be implemented under the supervision of a specialist.
How Is Bone Marrow Edema Treated?
Treatment is planned according to the cause, severity of the condition, and the patient’s overall health status. The main goal is to reduce the load on the bone, resolve the fluid accumulation, and improve the patient’s quality of life.
In most cases, non-surgical methods are preferred at the beginning. Rest and load reduction are recommended first. Reducing pressure on the affected area during daily activities helps stop progression and initiates the healing process. Avoiding sudden and strenuous movements is especially important during this period.
Ice therapy is often advised to control pain and inflammation. Ice helps reduce swelling and relieves localized inflammation. It also has a soothing effect on pain. Painkillers and non-steroidal anti-inflammatory drugs (NSAIDs) are prescribed as part of the medication plan. These drugs control inflammation and help patients perform daily activities more comfortably.
Supportive devices may be recommended for some patients. Canes, orthotics, or special braces help reduce joint pressure and protect the damaged area. These aids accelerate healing and lower the risk of complications.
With these measures, mild to moderate cases typically improve within 6 to 12 weeks. However, in some situations, conservative treatments may not be sufficient. If the condition reaches an advanced stage, standard treatments may become inadequate. In such cases, more comprehensive and specialized options may be required.

Frequently Asked Questions
Can it heal on its own?
Mild and early-stage cases can heal spontaneously. Rest, medication, and load reduction measures support this process. However, if the underlying cause is not treated, the condition may become chronic. This may lead to more serious problems.
Is MRI always necessary?
Yes. MRI is essential for a definitive diagnosis. Fluid accumulation inside the bone cannot be clearly detected with other imaging methods.
How long does the pain last?
The duration of pain depends on the severity of the condition and the response to treatment. In most cases, pain decreases significantly within 6 to 12 weeks. In advanced or chronic cases, this period may be longer.
Does every case require surgery?
No. Most cases improve without the need for surgery. Only severe conditions, such as avascular necrosis, may require surgical intervention.
Can it fully heal?
With proper diagnosis and appropriate treatment, full recovery is possible. However, early intervention is very important. Delayed cases carry a higher risk of permanent damage.
Can it recur?
Yes. If underlying risk factors are not controlled, it may recur. Re-injury can also increase the risk.
Can I exercise?
Exercise can be done under medical supervision with proper programs. However, unsupervised and excessive physical activity may worsen the condition.
How long does physical therapy take?
The duration of physical therapy depends on the severity and the patient’s condition. Typically, programs last 4 to 8 weeks. In some cases, treatment may take longer.
Is medication alone sufficient?
Medication helps control pain and reduce inflammation. However, it is usually not sufficient alone. It is typically combined with rest, physical therapy, and load reduction measures.
Which age groups are most affected?
It can occur at any age. However, athletes, older individuals, people with obesity, and those with metabolic disorders are at higher risk.
Conclusion
When diagnosed early and managed with appropriate treatment methods, this condition can largely be controlled. Especially in weight-bearing areas like the knees, hips, and ankles, it can significantly affect patients’ daily quality of life. In these regions, fluid buildup may lead to restricted movement. It can also cause constant pain and functional loss.
Therefore, individuals experiencing symptoms should consult an orthopedic specialist without delay. Early diagnosis is one of the most critical factors directly influencing treatment success. Specialists apply evidence-based approaches during treatment. They also develop personalized treatment plans tailored to each patient’s individual needs. This ensures that the most appropriate protocol is followed and increases the effectiveness of the process. Individually designed exercise programs and physical therapy applications are implemented. Advanced treatment options can shorten the recovery time. With proper management, the risk of recurrence can also be reduced. This risk can be brought significantly under control.
Bone marrow edema is a serious health issue that should not be neglected. If not treated in time, it may lead to permanent damage. Having accurate information and following expert guidance play a decisive role in the course of the condition.
For more detailed information on bone and joint health, visit our blog.